Body
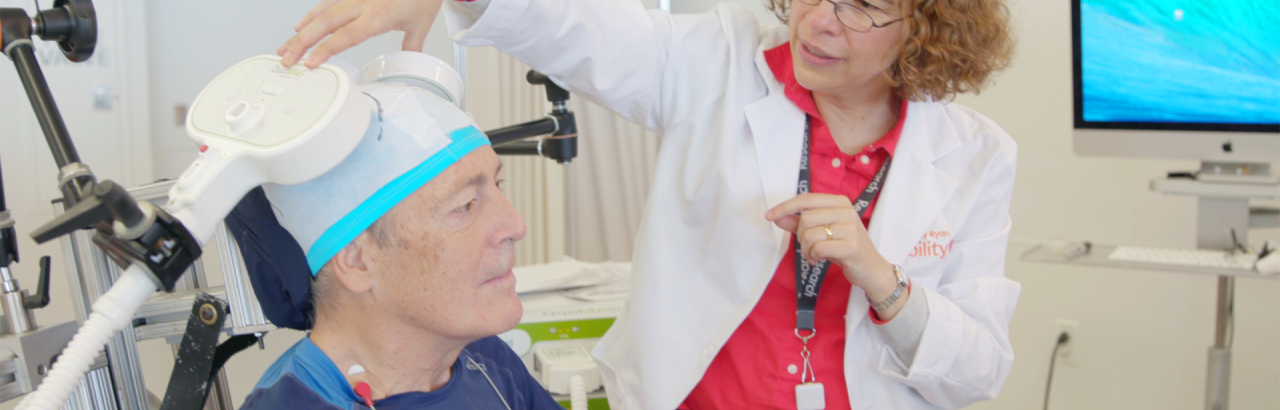
In novel research led by scientists at Shirley Ryan AbilityLab, patients with spinal cord injury who received non-invasive electrical stimulation simultaneously targeting motor neurons in the arms and legs followed by physical therapy had lasting improvements in walking and grasping. Their findings are reported in Annals of Neurology.
The work builds on previous studies also led by Monica Perez, PT, PhD, scientific chair of the Harris Family Foundation Arms + Hands Lab at Shirley Ryan AbilityLab and corresponding author on the paper. Dr. Perez and her team used a technique called Hebbian stimulation where neurons in the spinal cord and the motor neurons they connect to (those that innervate muscles) are electrically stimulated just microseconds apart through the skin. The technique, also known as paired electrical stimulation, or PAS, helps strengthen connections between spinal and motor neurons, improving the ability of signals to travel from the brain to muscles and cause movement.
In an initial study, 20 patients with spinal cord injury were randomly assigned to receive either 20 30-minute rounds of Hebbian stimulation targeting muscles in the legs followed by 60 minutes of physical therapy, or sham stimulation followed by physical therapy. They received treatment three to five times per week over the course of four to seven weeks. Compared with participants who received sham stimulation, those who received Hebbian stimulation showed greater improvement in walking speed and in the function of the neurons targeted.
“We saw patients who had difficulty moving their legs before the treatment take steps,” said Dr. Perez. “We wanted to see if even better outcomes could be achieved by increasing the number of sessions of Hebbian stimulation plus physical therapy, and we also wanted to see if we could see improvements in function in both the arms and legs using our protocol.”
Mentioned Profile

Monica A. Perez, PT, PhD
Scientific Chair, Arms + Hands Lab, Shirley Ryan AbilityLab | Professor of Physical Medicine and Rehabilitation, Northwestern UniversityBody
In a second study, 11 participants received 40 30-minute sessions of multi-site Hebbian stimulation targeting neurons that innervate both leg and arm muscles followed by 60 minutes of physical therapy. These participants showed significant improvements in their walking speed, corticospinal function, grasping and in overall quality-of-life measures. They maintained some of these improvements nine months after therapy.
The research found that more stimulation led to better outcomes. Compared with patients who had physical therapy alone, patients who underwent 20 sessions of Hebbian stimulation had a 70% improvement in walking speed and patients who had 40 sessions of Hebbian stimulation had a 125% improvement in walking speed. Quality-of-life measures also improved in patients who underwent 40 sessions of the protocol.
“Dr. Perez was very interested in looking beyond the physiological effects of her intervention to understand how the treatment might affect quality of life for participants in the study,” said Allen Heinemann, PhD, Director of the Center for Rehabilitation Outcomes Research at Shirley Ryan AbilityLab and a co-author on the paper.
As part of the study, Dr. Heinemann suggested a patient-reported instrument that measures ambulation, self-care, toileting and physical-mental health. Patients who underwent 40 sessions of Hebbian stimulation reported functional improvements in self-care and toileting but some of these improvements returned to baseline at nine months after treatment ended.
“For the first time, we used our stimulation technique at multiple sites to target different muscle groups, and we saw that patients who received this treatment together with exercise showed clinically significant improvements in function, including walking and in grasping,” said Dr. Perez, who also is a professor at the Northwestern University Feinberg School of Medicine and research scientist at the Edward Hines Jr. VA Hospital. She is looking forward to reporting on further studies that look at improvements in function beyond 40 sessions of Hebbian stimulation. “We have not yet identified a plateau in terms of functional improvement with increased number of sessions.”
This research was funded by the National Institutes of Health, Veterans Affairs and the Walkabout Foundation.
To reach the full study: https://pubmed.ncbi.nlm.nih.gov/36843340/
Mentioned Profile