Body
Non-invasive Neurostimulation Paired With Physical Therapy Temporarily Mends Broken Connection Between Brain and Spinal Cord in Patients with Spinal Cord Injury
Amber Bruce, 33, an Atlanta resident and sports marketing professional, became almost completely paralyzed when she inexplicably fainted on Jan. 31, 2019. Since then, she has worked tirelessly to regain function and ability through physical therapy and participation in clinical trials. However, not until she participated in a study at Shirley Ryan AbilityLab has Amber, who was initially told she would never walk again, made such tremendous progress. After 40 sessions of non-invasive neural stimulation, followed by an hour of physical therapy each time, she took her first steps. By the end of the treatment protocol, two-and-a-half months later, she could take more than 60 steps.
For the first time, this research — led by Monica A. Perez, PhD, PT — has demonstrated that this non-invasive neurostimulation treatment that targets synaptic connections in the spinal cord improves and preserves physical therapy functional improvements in patients with spinal cord injury — temporarily mending the broken connection between the brain and spinal cord. Findings have the potential to help the approximately 294,000 people in the United States who live with spinal cord injuries.
“When a patient has a spinal cord injury, the communication link between the brain and body is damaged, leaving them functionally unable to communicate with each other,” said Dr. Perez. “The effect is like a telephone wire that has been cut: two parties are talking, but each side can’t hear what the other is saying. Our goal is to understand if we can strengthen connections in the spinal cord by targeting residual pathways from the brain and peripheral nerves that are still available after spinal cord injury, and try to maximize their interactions.”
Body
Several previous studies have found that rehabilitation can be augmented by neurostimulation, but these studies used protocols with limited or short-term results or used invasive approaches. Now, Dr. Perez’s novel non-invasive neurostimulation technique — paired with physical therapy — has been proven to maximize clinical outcomes in patients with spinal cord injury for at least six months. Dr. Perez’s group is the only one in the United States using this approach to target spinal synapses in patients with spinal cord injury.
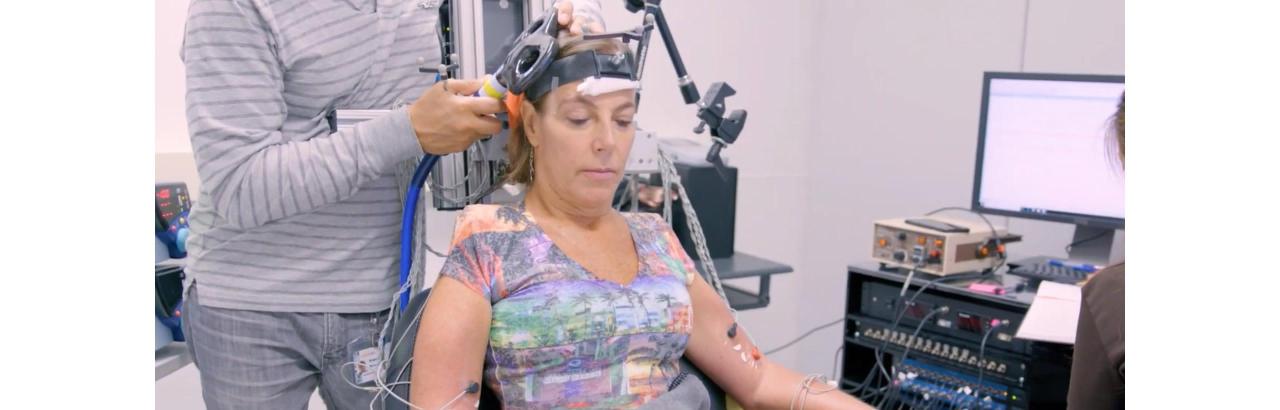
With this treatment, called paired corticospinal-motoneuronal plasticity (PCMS), targeted electric pulses stimulate the subject’s brain and send motor neuron signals down toward the body; the signals inevitably stop at specific times at the area of the spine that is injured. Concurrently, electric pulses send motor neurons through the peripheral nerve up from the targeted area of the body, also reaching the point of injury in the spine. The key breakthrough of PCMS is in ensuring the volleys elicited by neurons reach the spinal cord in a precisely timed manner. This coordination effectively mimics a complete communication circuit between the brain and body based on fundamental principles of neuroplasticity.
“The timing for this plasticity is very important,” said Dr. Perez. “We do not just randomly stimulate the brain or the peripheral nerve. Instead, we use electrophysiology to measure the transmission times from the brain to the spinal cord, and the muscle to the spinal cord. The science has evolved so much that we can make those estimations.”
To date, more than 60 subjects with chronic incomplete spinal cord injury have participated in Dr. Perez’s studies at Shirley Ryan AbilityLab. They are randomized into groups that receive sessions of physical therapy for 45 minutes after 30 minutes of targeted PCMS, or sessions of therapy for 45 minutes after a sham PCMS. An additional experiment tests the effect of PCMS without therapy in a similar cohort. The targeted neurostimulation protocol has been customized to include patients with different levels of injury (cervical, thoracic or lumbar). Researchers take measurements before the intervention, immediately following the intervention and then six months later.
They’ve found that corticospinal excitability and the magnitude of maximal voluntary contractions in targeted muscles increase by 40-50% after PCMS with or without therapy, but not in the sham experiment. Individuals in the experimental group who also undergo physical therapy improve their walking speed and are able to grasp different objects more quickly. Dr. Perez’s research is the first to show that functional gains can last for at least six months — a truly dramatic result for this patient population.
The Next Step
Spinal cord injuries are different for each person — based on what part of the spine was damaged and the severity of the injury.
“That is why we made our protocol flexible,” said Dr. Perez. “We can adapt it and elicit the same type of plasticity in different muscle groups.”
For the next phase of research — which is now recruiting subjects — Dr. Perez is applying stimulation to the brain and more than one peripheral nerve simultaneously, targeting sensory and motor fibers. Research subjects will undergo this treatment, combined with physical therapy, across 40 sessions at Shirley Ryan AbilityLab. It’s the next step in a progression building on years of tested and perfected neurostimulation techniques, and Dr. Perez says every indication is that more promise lies ahead.
“We are seeing no plateau in patient results,” she said. “There's much to understand yet, but it is promising.”
As for Amber, who has since returned to Atlanta, she remains determined to continue on this trajectory and hopes to continue with the study.
“I am going to improve,” said said. “I am going to walk.”
Mentioned Profile