Body
Parkinson's disease causes progressive mobility deficits associated with decreased quality of life and increased mortality. European clinical practice guidelines recommend physical therapy (PT) for people with Parkinson’s disease (PD) soon after diagnosis to provide education, physical activity advice, and individualized interventions when needed. However, PT is frequently under-utilized early and individuals aren't referred until gait and balance problems occur. The purpose of this administrative case study is to present the application of a proactive PT (PAPT) approach, to optimize participation in evidence-based exercise for PD, using implementation frameworks for the (1) implementation process, (2) determinants of implementation success, and (3) implementation evaluation.
Description of Study Activities
Body
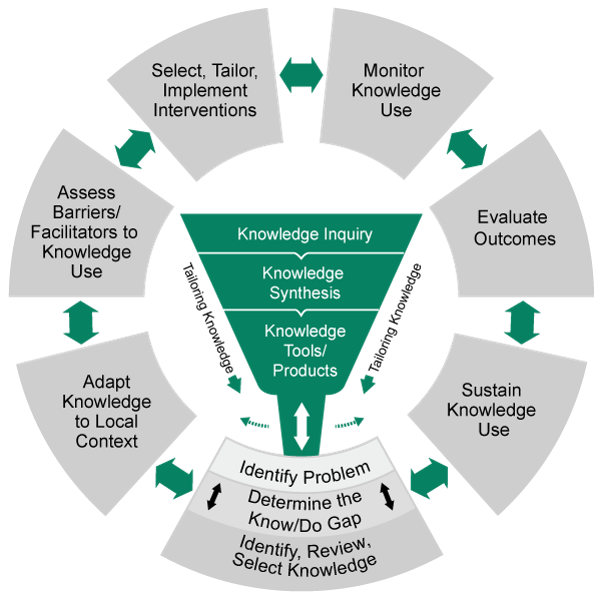
The PAPT program targets people with early stage PD before the onset of significant gait and balance dysfunction. The program uses a shared decision-making model to promote long-term maintenance of independent exercise. The Knowledge-to-Action Framework was used by champions to assess gaps between knowledge and current practice as well as synthesize current knowledge regarding exercise in PD. Implementation barriers were addressed using the Consolidated Framework for Implementation Research.
The PAPT program was initiated in January 2016 and evaluated using the RE-AIM (Reach, Effectiveness, Adoption, Implementation, Maintenance) framework with mixed methods. Project 1 has been completed and accepted for publication.
A second cycle through the Knowledge-to-Action Framework cycle was initiated in 2018 related to the spread and sustainment of the PAPT program through a regional rehabilitation system of care. The analyses are underway.
Project 1 Results
Body
In the program’s first year, 38 people were referred, 28 were evaluated, and 20 participated in 6 month program evaluation. After the first session, individuals followed 1 of 4 care paths to provide individually tailored intervention. Following PAPT, the number of participants reporting regular participation in aerobic, strengthening, flexibility, and balance exercise increased. Participants reported a median of 140 of aerobic exercise per week. Implementation barriers included location, insurance coverage, and difficulty scheduling long-term follow up visits. Participants reported physical and emotional benefits of the program. Referral rates increased from targeted referral sources by 55-163%.
Project 2 Preliminary Results
Body
In the program’s first year, 26% of referred individuals (10 of 38) did not attend the urban program due to barriers due to lack of value of the program given interest, transportation, or cost barriers. During the first year of program expansion, our PTs reached 61 patients, and we are on target for additional growth in 2019. Key barriers in suburban programmatic development include slow referral growth, staff turnover, and scheduling communication. Unique benefits of implementing a program the smaller clinical settings include completion of patient-reported outcome measures, better consistency of therapists with smaller programs. The most potent facilitator of program sustainment were administrative and leadership support. Knowledge broker and champions collaborated to address barriers to develop a program at each site.
