Project Overview
Body
Principal Investigator: Arun Jayaraman, PT, PhD
Co - Investigator: William Zev Rymer, MD PhD
Synopsis/Goals of the Project
As exoskeleton devices become more prevalent and begin to be available for personal use, there must be consensus on training strategies for safety and independence in exoskeleton ambulation. While there are limited studies of indoor level ground use, there are no studies examining stairs, ramps, or outdoor un-level ground ambulation. Furthermore, there is no consensus on the criteria for independent ambulation in exoskeletons. Therefore, this study will both identify the level of competency necessary in various skills for independent use of the ReWalk as well training strategies for this end.
Primary objectives:
- To determine the training program necessary for independent use of an exoskeleton for ambulation over level and un-level surfaces including stairs, ramps, curbs and outdoor surfaces.
Secondary Objectives:
-
To develop an objective evaluation of competency for safe and independent use of an exoskeleton for ambulation over level and un-level surfaces including stairs, ramps, curbs and outdoor surfaces.
-
To identify the physiological and psychological predictors of ideal candidates for everyday exoskeleton use.
Major Accomplishments
Body
The optimal protocol for exoskeleton-assisted gait therapy
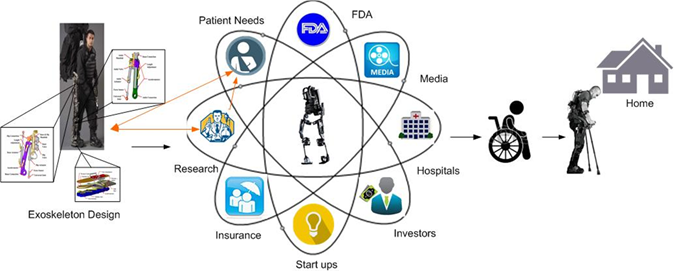
Powered robotic exoskeletons are an emerging technology of wearable orthoses that can be used as an assistive walking device in individuals with lower limb paralysis and/or as a therapeutic tool to improve independent ambulation. Several versions of exoskeletons have been in development over the past few years. Since the beginning of the project, we have worked with the RewalkTM (Rewalk Robotics), the EksoTM (Ekso Bionics) and the Indego® (Parker Hannifin Corporation).
Our laboratory has close association with these three exoskeletons since their inception into clinical research in provide valuable feedback to the field of Rehabilitation Robotics. The data collected during our various clinical trials was instrumental in securing FDA approvals of these devices in certain neurological conditions, namely Stroke and spinal cord injury.
In a recent clinical trial with Rewalk in individuals with chronic spinal cord injury, where we trained the participants, three times a week up to 36 weeks. To our understanding, it was a better training paradigm for optimal learning. More than 18 training sessions are needed for
Independent use of the device, especially for skills dealing with community barriers of ramps, curbs, stairs. None of our subjects had plateaued in their learning after 18 sessions. Studies of this type are needed to identify appropriate patients (with respect to injury level, severity of disability) and to bring out the true potential of these robotic exoskeletons.
The data we collected using the ReWalk has since transcended to two home trials and triggered multi-center clinical trials. In these trials we are gathering data not only on usage of the device, but also physiological parameters that may improve such as those that could be seen with a pulmonary function test, ECG, CT scan, and bone density scans to establish any potential health benefits due to exoskeleton use. Based on our successful implementation of this project, we are able to expand our ability to serve the industries in developing exoskeletons that are more effective. Currently more than 12 exoskeleton companies are in collaboration with our laboratory.
The questions that still need focus are in regards to timing of training and therapy. In a new pilot study, we intend to target individuals with spinal cord injury during their early recovery process by subjecting them to exoskeleton training. Individuals with less than 6 weeks post injury are given exoskeleton training along with functional electrical stimulation (FES) to obtain significant improvement in their walking ability. Improvements are tracked via MRI scanning and weekly ASIA testing.
For more detailed information (scientific publications, etc.):
Abstracts:
-
Hohl K & Jayaraman A. Panel Presentation. Incorporating exoskeletal robots into clinical practice. American Academy of Physical Medicine and Rehabilitation Meeting, New Orleans, November 2016.
-
Hohl K & Jayaraman A. Talk. Exoskeletons: Powering Up Rehabilitation. Midwest chapter of the American academy of Orthotists & Prosthetists, Rosemont, IL, November 2016.
-
Forrest G, Kozlowski A, Tefertiller C, Jayaraman A, Kandilakis C. Symposia. Exoskeleton-assisted walking for persons with neurological conditions. Case series American College of Rehabilitation Medicine. Chicago, IL, November 2016.
-
Holh K, Minarsch R, Scanlan K, Mummidisetty K, Jayaraman A. Is a structured exoskeleton overground gait training program superior to traditional care in individuals affected by chronic severe stroke? Poster. Combined Sessions Meeting, San Antonio, TX, February 2017.
-
Tefertiller C, Jayaraman A, Forrest G, Hartigan C. Initial Outcomes from a Multi-center Feasibility Study Utilizing the Indego Powered Exoskeleton in Spinal Cord Injury. Oral Presentation. ASIA Annual Meeting, Albuquerque, NM, April 2017.
Invited talks:
-
Jayaraman A. Plenary Speaker. APTA Section on Neurology and Pediatrics IV STEP Joint Conference. Technology Use for Plasticity and Participation. Columbus, Ohio, July 2016.
-
Jayaraman A. Invited Speaker. Wearable Technology and Remote Monitoring. Miles Square Health Center & Breathe Chicago, University of Illinois at Chicago, July 2016.
-
Jayaraman A. Invited Speaker. Wearable Robotics: A chance to walk from the clinic to your home. Rehabilitation Science Seminar Series, University of Florida, Gainesville, FL, September 2016.
-
Jayaraman A. Invited Speaker. Exoskeletons for Rehabilitation & Personal Mobility: Creating Clinical Evidence. The International Symposium on Wearable Robotics. Segovia, Spain, October 2016.
Review Articles:
-
Esquenazi A, Talaty MM., Jayaraman A. Powered Exoskeletons for Walking Assistance in Persons with CNS injuries. A Narrative Review. PM&R Journal August 23rd 2016
Mentioned Profile


