Body
Doctors define and describe spinal cord injury (SCI) using a system of numbers and letters that align with various sections of the spine and spinal cord.
Components of the spinal cord
Body
The spinal cord is a dense bundle of nerves that runs through a canal created by the protective bone segments of the spine (vertebrae). It travels downward from the base of the brain, through the middle and lower back to the “tailbone.” Even where the spinal cord ends, spinal nerve roots continue to run from the end of the cord to the lower spinal canal.
Your brain and spinal cord form part of the nervous system. The brain is the command center, and the nerves in the spinal cord are the pathways that make it possible for the brain and the body to communicate. Typical messages include controlling the movement of our muscles, the ability to feel (sensation), and some automatic functions of our body (e.g., breathing, heart rate, among others).
Impact of SCI on the body and function
Body
When the spinal cord is injured, that communication is interrupted or prevented, depending on the severity of the injury and where it is located on the spinal cord.
The spine and spinal cord are divided into sections or “levels.” The vertebrae are named and numbered to correspond with the various functions associated with that part of the spinal cord. There are five levels, staring at the top and going downward: Cervical (C), Thoracic (T), Lumbar (L), Sacral (S) and Coccygeal (Cx).
These main sections include a group of vertebrae, each of which is given a number that increases as you move down the spine. So, from top to bottom: C1–C7; T1–T12, L1–L5, S1–S5, Cx3–Cx5. 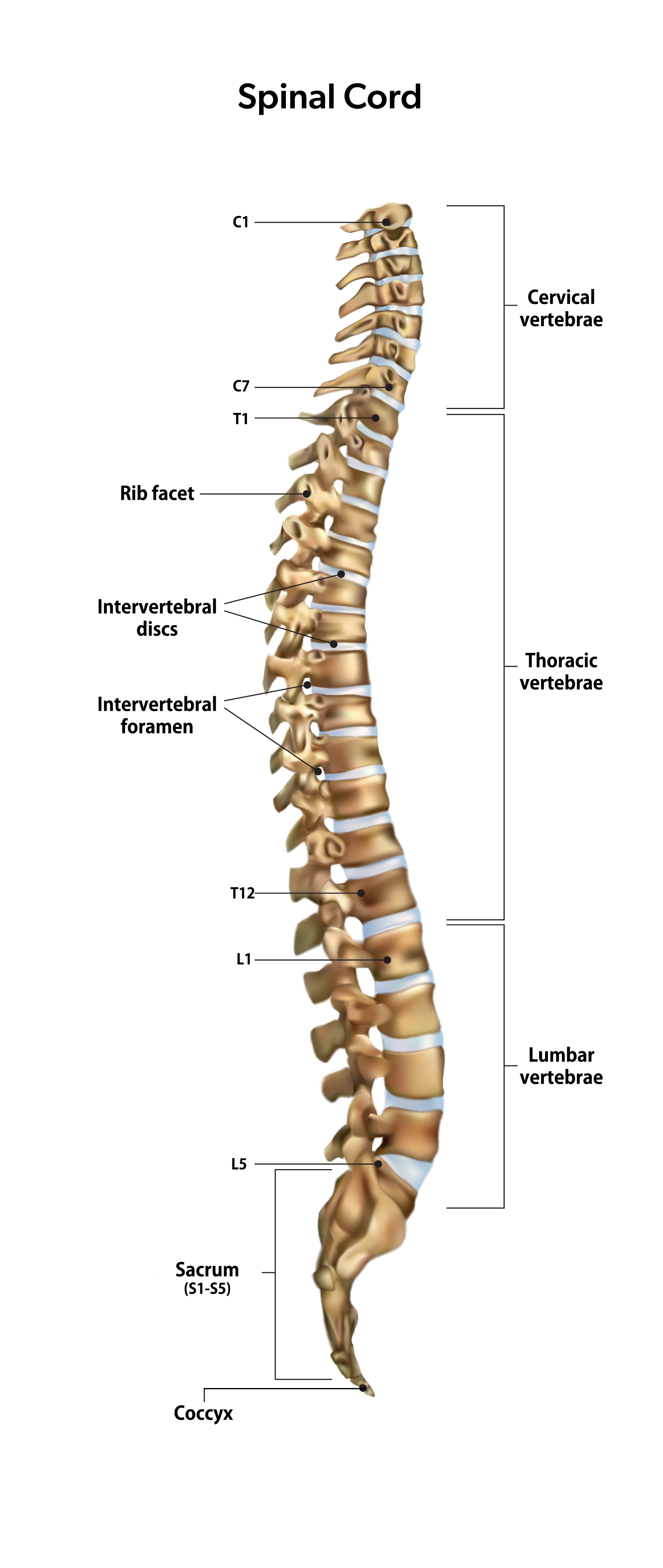
Assessing a spinal cord Injury
Body
The American Spinal Cord Injury Association (ASIA) has created an exam that is given to people with injuries to the spine and/or spinal cord. The ASIA exam is a system of tests used to define and describe the extent and severity of someone’s spinal cord injury. The results of the exam can guide rehabilitation and recovery needs.
The ASIA exam determines the point on the spinal cord below which the feeling (sensory function) and ability to move (motor function) are affected, as well as how severe the impact is.
The link between SCI level and loss of function
Body
In general, the higher the injury on the spinal cord, the more sensation and function are affected. In other words, the degree of “paralysis” (loss of ability to feel and move) is related to the location of the injury. Injuries to the upper portion of the spinal cord may cause “tetraplegia” (paralysis of upper and lower body). Injuries at the bottom of the spinal cord may cause paraplegia (paralysis of the lower body).
What is the difference between “complete” and “incomplete” SCI?
Body
An SCI is considered “complete” when no control signals from the brain are making it all the way down to the very end portion of the spinal cord (rectal area). If there are none, then there will usually be no sensory or motor function between the location of the injury and this point.
An SCI is considered “incomplete” when some signals are getting through to the end point, but not all. In this case, changes in sensation and motor function will correspond with the location of the injury. With incomplete SCI, there will be some feeling and ability to move below the point of injury.
How much function will return after SCI?
Body
Although there is no way to tell for sure how much function will return, potential for recovery can be based on whether an injury is complete or incomplete. It is very possible for function to improve, even if severity does not.
Find more information on recovery from spinal cord injuries.